by The Chronic Chronicles | Dec 23, 2013 | Hospitals
I stumbled across the treatment of ‘infusions’ sometime ago, and then kept seeing them being mentioned. I began to try to find out more about them, but information was limited.
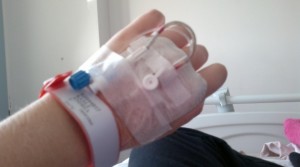
I was aware it usually consisted of either Ketamine or Lidocaine being given by an IV, and for some it works really well for pain relief. For others it seems to do nothing at all.
Eventually a friend kindly offered to search the academic databases he had access to and sent me all the research he could find. They were generally all positive.
‘Intravenous Lidocaine: An Outdated or Underutilized Treatment for Pain?’ by Gary McCleane stated, “The drug is administered over a relatively short period of time and yet the potential relief lasts significantly beyond both the period of administration and the plasma half-life of this local anesthetic.” He goes on to state that, “an infusion over a few hours can produce relief that extends to weeks and even months. Consequently, side effects, if any are apparent, are short lived and last for a much shorter time than the pain relief.”
McCleane explained that for many patients undertaking this treatment it becomes their only form of pain-relief, and they’re able to stop all other medications for pain. A trial of 82 patients found that 82% had a very good pain reduction after their infusion. In a second study on people with Fibromyalgia it was found that 40% of patients had between 13-18 weeks of relief.
A second study called ‘Efficacy and adverse effects of intravenous lignocaine therapy in fibromyalgia syndrome’ concluded that the therapy “appears to be both safe and of benefit in improving pain and quality of life for patients with fibromyalgia.”
The one downside is that there wasn’t much research on the therapy, and when a study had taken place they had very small sample sizes. There are also side effects such as hypotension, tachycardia, infections and other such fun times.
I began by asking my GP about them, but she’d never heard of them. I asked at the various London hospitals I’m under, but was told they didn’t do them. I came across a number of people with Ehlers-Danlos Syndrome who’d had them, but it was never at a hospital near to me.
I then visited a pain clinic in another town but they too stated they didn’t do them, and if they did they wouldn’t do it for Ehlers-Danlos Syndrome as there weren’t enough of us with it. (Red flag to a bull!)
I then changed GPs, and she too hadn’t heard of them – but a few weeks later I got a phone call from her. She explained she’d just had a patient in to see her who’d just had infusions at the hospital in my own town! She told me to come and see her, and she’d get me referred.
I saw a consultant at the pain clinic last week and she agreed I could have one infusion. I’m not sure why just one, but still it’s good news!
I’m also due to have facet joint injections in January, so there are two treatments coming up that allow me to have some hope.

An IV
Credit to: andyk

by The Chronic Chronicles | Dec 16, 2013 | Coping Methods
When you’re in constant pain, it’s very easy to focus on it. It can become all-consuming, and the more you think about it – the worse it feels. Someone once suggested to me that I try crafting as a means of distraction. I have to be honest, I was a little annoyed – how would painting a pretty picture take my crippling pain away? It seemed a little dismissive. Plus there was also the fact I’d never thought of myself as a particularly creative or artistic person. At school even my doodled stick figures ran screaming in terror, and my art teacher made it clear it wasn’t my forte, but I thought I’d give card-making a try.
I enjoyed making them, but they weren’t that great. I’d look online at all the beautiful designs people were creating, and it just didn’t feel quite like me. After I’d spent a fortune on card-making supplies, I decided to try my hand at jewellery instead, and in doing so found a new passion.

Stargazer Watch
The early days of making jewellery weren’t easy – my hands cramped up terribly, and I was left with blisters all over my skin. In time my dexterity improved and it helped strengthen some of my muscles in my hands. And it was true – when I’m busy concentrating on making a new item, my brain is focused elsewhere. It doesn’t make the pain go away, it just redirects my attention so I’m not thinking about it, which is really helpful.
Once I joined the world of crafting – I found more and more other people with disabilities were also there, and finding an outlet in art – by painting, woodwork, ceramics, photography or anything in-between. For example a friend of mine makes ‘pain monsters’ from felt when she’s having a bad day, which helps her create a visual representation of what she’s feeling.
It took me quite a long time to find out what was wrong with me. Many years of fighting and pleading with the medical community to stop shrugging their shoulders, and to do something. When I was told I had Fibromyalgia, it came as something of a relief. I felt like I wasn’t alone – there were other people with this stupidly long list of symptoms out there. I wanted to commemorate the end of that fight, that also informed people about the condition. I made my first Fibromyalgia awareness bracelet not long after, and then began to receive requests to create ones for other conditions – including some I’d never heard of before. People liked the more personalised feel to the more generic rubber bands that are usually sold. My biggest seller was for Marie Charcot Tooth Disease, and eventually the national charity began to order from me so they could sell them on their website.
I also auctioned lots of my bracelets off for the Fibromyalgia Association UK, and also for Ehlers-Danlos Syndrome related charities when I was diagnosed, a genetic multi-systemic connective tissue disorder. It made me feel like I was helping, even in one tiny way.

An Ehlers-Danlos Syndrome bracelet featuring zebra stripe beads – the symbol of the condition
It’s very common to walk into a shop and see a row of pink coloured items for Breast Cancer awareness. Yet there are so many other conditions that people often haven’t even heard of before, let alone understand what they entail and what it’s like to live with them. People have often told me when wearing one of my awareness bracelets it has sparked conversations with friends and family who had never asked about their health before.

Fibromyalgia Awareness Bracelet

Fibromyalgia Awareness Bracelet 2
The colours of the bracelets are usually picked by the existing awareness ribbon colour, and if there isn’t one, then by the colours of the national organisation/charity for the condition. Sometimes there are obvious symbols that can be included as charms. Fibromyalgia often has an association with butterflies, Autism with jigsaw pieces, Charcot Marie Tooth Disease with hands and feet. Sometimes a spoon charm is added from the fantastic analogy “The Spoon Theory” by Christine Miserandino, to which many people with chronic illness resonated with. My most commonly used charm is simply a silver ribbon with the word hope written on it – as I believe that’s something we all need in some form or another.

Arthritis Awareness Bracelet
In April this year I had to stop working due to my health continuing to get worse. Being able to make jewellery – even if it’s for twenty minutes in the middle of the night when I’m struggling to sleep, has helped keep my spirits up and creativity flowing.
If you’re interested in seeing more of my jewellery and awareness items you can find me under Sparkly Place Jewellery on Facebook.

by The Chronic Chronicles | Oct 22, 2013 | General Posts

Living Well with Fibromyalgia is an online magazine written by and for people with the condition, and published by the fabulous website FibroModem. They are currently looking for people who would like to appear on the cover. It’s a great way to represent the normal people living with the condition, as well as get your chance to be a star!
You need to submit your photo by the 1st November to contributions@fibromodem.com. Full terms and conditions can be found here.
Good luck!

by The Chronic Chronicles | Aug 3, 2011 | Coping Methods, Diagnosis
My pain started when I was 10, and has been constant since I was 15. I saw doctor after doctor and got nowhere.
Some said I’d grow out of it, others seemed to content to tell me it wasn’t arthritis, and send me on my way.
I just wanted to know what it was. I needed to put a name and I pleaded with them for one, but was told they didn’t want to ‘label’ me. I was in non-stop, agonising, soul-destroying pain. I couldn’t go out with friends, I was exhausted and felt completely alone. I thought knowing the name of my condition would make me feel like there were others out there just like me. I didn’t see how it was a label – it was the name of my bloody condition, and I wanted to know what it was.
In 2005 I was told by a rheumatologist I’d grow out of it. In 2008 I got really pissed off, and saw three consultants. In March it was due to subluxation, in July Chronic Myofacial Pain and by August it was simply ‘mechanically related’. What the hell did they mean? They were wishy-washy nothingness!
I was at university one day, and was probably putting off writing an essay, when I put every single one of my symptoms into google and hit search. A condition called Fibromyalgia popped up.
I read down the list and read everything I could about it. It fit me! Everything it said I could relate to. The relief was – I can only describe it as immense. I didn’t even register the bit at the bottom that said it was incurable.
I hit print and phoned my doctors, and made an appointment for that day. It was a doctor I’d never seen before, as I’d fired my previous GP for using the unforgivable phrase.*
I remember the GP finally asking for my symptoms that day. Do you know how rare that it? Most get to pain and stop there, as if the hundreds of other crap that goes alone with it means nothing. He nodded and said yes, it does sound like Fibromyalgia – but you need a clinical diagnosis and so sent me to a Pain Clinic, who still did not give me a diagnosis – but gave me nine facet injections in the facet joints of my neck, and muscles of my shoulder.
It took until January this year – eight years – until I finally ‘hit the jackpot’ by getting some decent doctors and some actual diagnoses. I saw two specialists on the same day, one who diagnosed me with Fibromyalgia, and the other with Ehlers-Danlos Syndrome (and lots of related conditions).
So, I’ve completed the battle in getting the names, and it did help. When people ask what’s wrong, I can tell them rather than shrug my shoulders. I can meet people in the same boat and keep on top of research.
But where do I go from here? My pain hasn’t improved, and in fact gets worse all the time. My lower back seems have gone on the warpath to unbearable levels, and my McTimoney Chiropractor, who usually has magical powers in finding the culprit and sorting it out, even temporarily, hasn’t been able to touch the problem.

Credit to Dennis Taufenbach
Do I keep battling on? Do I keep asking to see new professors who I hear have helped others? Before I got my diagnosis I was going to ask to see an Orthopaedic doctor to try and see if they could do anything with my lower back, but now I have been told I have Ehlers-Danlos Syndrome and Fibromyalgia, are they just going to shrug and say well you have those, what do you expect? Or might they be able to do proper scans and sort out some of the pain? I just don’t know. I feel a bit lost, and am not sure where to turn.
I am on the waiting list for intensive in-patient treatment at the Royal Orthopaedic hospital in Stanmore, for pain management, but it’s still not looking into causes and fixing it.
I guess what kept me going was finding out what’s wrong with me, and now I do, I wonder if this is it?
* The unforgiveable phrase is ‘there isn’t a magic wand that can cure you.’ Did I ask for a magic wand?! No! Just a doctor that does their best to help. That’s all.
by The Chronic Chronicles | Jul 15, 2011 | Daily Life
Karen Lee Richards has written the top then things never to say to someone with Fibromyalgia here. Her list, my thoughts. She has more at the link.
10. We all get more aches and pains as we get older.
My pain started when I was about 10, and hasn’t stopped since I was 15. I’m not old. It’s so much more than aches and pains. An old lady shivered the other day and said she felt the cold. I agreed I did too. She glared telling me to wait until I was older. Right.
9. I think I have that, too – I’m always tired.
It’s not just tiredness. It’s crippling fatigue. I’m lucky in that generally I have a lot more of the pain than the fatigue, and I do take a lot of steps to try and pace myself. The second I don’t – I’m screwed up for days. It’s bone aching exhaustion and there’s nothing you can do about it.
8. My friend has fibromyalgia and still manages to work. Maybe you just need a job (hobby, etc.) to take your mind off the pain.
I am currently working three days a week. I work a day, have a day off. I’m off sick a lot, and am struggling my arse off to carry on, because I just can’t afford not to work. It doesn’t mean I’m not bad, I just feel at the moment, I don’t really have a choice.
7. My doctor says fibromyalgia isn’t a real disease; it’s just a wastebasket diagnosis.
Utter rubbish. Sadly a lot of doctors don’t keep up with the research, and still see it as ‘I don’t what else you’ve got so I’ll say you have fibro.’ There is lots of evidence it exists. At consultant at the local hospital said I had it, but refused to officially diagnose me as it was too “American.” If by that he means they take it a bit more seriously, then sure. But the illness is real and debilitating as any other, and has no nationality.
6. If you got more sleep, you’d feel better.
I do sleep. I can sleep up to 16 hours sometimes, but other times struggle to sleep four. But no matter how many hours I wake up exhausted, because people with Fibromyalgia do not reach the ‘deep sleep’ stage, the restorative and healing stage. So the problem is our sleep has no quality to it, it doesn’t really matter how much you get.
5. I read about this new product that cures fibromyalgia.
Yeah? How much does it cost? It’s amazing how many new products come out that totally cure x y and x, but whoops, it costs £1000+. I’ve heard so, so many therapists tell me they can cure me and then not make the slightest bit of difference. If a product genuinely works, I find most people want it to reach as many people as possible at a cost they can afford. Generally.
4. At least it’s not fatal.
But it has changed my life. It took away my ability to walk, to fully enjoy socialising, to work how I wish. Sometimes during my worst days I do wish it was fatal because it’s hard not to when you’re constantly exhausted and in agonising pain. I believe conditions like this should be taken just as seriously as fatal ones, because they truly impact every facet of your life and if it was taken seriously hopefully more resources could be put into research.
2. But you don’t look sick.
That’s because you don’t see me when I wake up almost screaming in pain because some joint is out of place. You can’t see pain visually, but you can if you pay attention.
1. It’s all in your head.
Yeah, something probably has gone wrong in our head like our brain is recognising pain signals far too much, but it’s totally and utterly real.

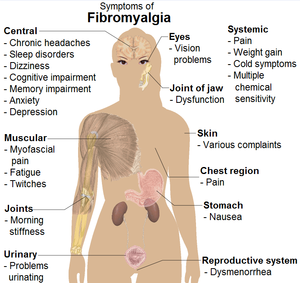
Common signs and symptoms of fibromyalgia.(Photo credit: Wikipedia)









