by The Chronic Chronicles | Dec 23, 2013 | Hospitals
I stumbled across the treatment of ‘infusions’ sometime ago, and then kept seeing them being mentioned. I began to try to find out more about them, but information was limited.
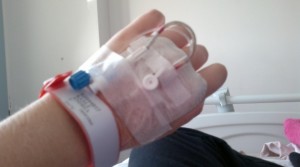
I was aware it usually consisted of either Ketamine or Lidocaine being given by an IV, and for some it works really well for pain relief. For others it seems to do nothing at all.
Eventually a friend kindly offered to search the academic databases he had access to and sent me all the research he could find. They were generally all positive.
‘Intravenous Lidocaine: An Outdated or Underutilized Treatment for Pain?’ by Gary McCleane stated, “The drug is administered over a relatively short period of time and yet the potential relief lasts significantly beyond both the period of administration and the plasma half-life of this local anesthetic.” He goes on to state that, “an infusion over a few hours can produce relief that extends to weeks and even months. Consequently, side effects, if any are apparent, are short lived and last for a much shorter time than the pain relief.”
McCleane explained that for many patients undertaking this treatment it becomes their only form of pain-relief, and they’re able to stop all other medications for pain. A trial of 82 patients found that 82% had a very good pain reduction after their infusion. In a second study on people with Fibromyalgia it was found that 40% of patients had between 13-18 weeks of relief.
A second study called ‘Efficacy and adverse effects of intravenous lignocaine therapy in fibromyalgia syndrome’ concluded that the therapy “appears to be both safe and of benefit in improving pain and quality of life for patients with fibromyalgia.”
The one downside is that there wasn’t much research on the therapy, and when a study had taken place they had very small sample sizes. There are also side effects such as hypotension, tachycardia, infections and other such fun times.
I began by asking my GP about them, but she’d never heard of them. I asked at the various London hospitals I’m under, but was told they didn’t do them. I came across a number of people with Ehlers-Danlos Syndrome who’d had them, but it was never at a hospital near to me.
I then visited a pain clinic in another town but they too stated they didn’t do them, and if they did they wouldn’t do it for Ehlers-Danlos Syndrome as there weren’t enough of us with it. (Red flag to a bull!)
I then changed GPs, and she too hadn’t heard of them – but a few weeks later I got a phone call from her. She explained she’d just had a patient in to see her who’d just had infusions at the hospital in my own town! She told me to come and see her, and she’d get me referred.
I saw a consultant at the pain clinic last week and she agreed I could have one infusion. I’m not sure why just one, but still it’s good news!
I’m also due to have facet joint injections in January, so there are two treatments coming up that allow me to have some hope.

An IV
Credit to: andyk

by The Chronic Chronicles | Apr 2, 2013 | Coping Methods
I’m not a morning person.
At all.
So I find it slightly…irritating, I have to get up early in order to go to the relaxation sessions I’ve been having over the last few weeks. I don’t find that relaxing at all!
Relaxation sessions is one of the treatments the local pain clinic offers. To be fair – the clinic doesn’t offer that much, but the relaxation sessions are one of the handful of treatments they do. They’re run by a friendly nurse, in a room that hasn’t changed in the ten years I’ve been going to the pain clinic, the chairs are uncomfortable, and it’s kind of cold. But they do offer pillows, of which I usually take about five just to get to basic levels of the chair not completely sucking.
Relaxation is a funny one. I don’t tend to do it at home, because if I do I just fall asleep. The one time I remember it being successfully done at home was on a lovely summer day, and I dragged my yoga mat outside and lay listening to the peace and quiet, the sun warming me up and my laptop playing the free CD the pain clinic gives at the end of the sessions.
I do hope to do it again this summer, but generally I’m always too busy doing… something, and don’t make time for relaxation like I should.
When you have chronic pain, it’s generally thought the natural fight or flight response to the body has gone a bit haywire, and it’s constantly in fight mode. You’re naturally stressed, your nerves are constantly firing in pain and your muscles tense up. Relaxation is aimed at trying to break this connection between the brain and the body, to try and release those muscles and to de-stress.
I generally don’t find any benefits of relaxation last long-term, but I do find it a good distraction when I take the time to do it – and find I do achieve a deep relaxation where I have no idea what’s happening, which is always a plus!

Sometimes when in pain it’s also an idea to concentrate on your breathing – by putting your hand on your abdomen and slowly breathe in and out, trying to push your breath down as far as possible – instead of breathing in the chest like most people do as a bad habit. Again, I find this does reduce pain a little sometimes, and calms me – and again works well as a distraction technique.
My last session with the pain clinic is tomorrow, but if it’s something that interests you I’ve found my local Health In Mind (http://www.rethink.org) offer similar free sessions, or it’s something easily done yourself by downloading a relaxation track, or for free on YouTube.
Where you’re favourite place to relax? How often do you fit it in?

by The Chronic Chronicles | Feb 1, 2013 | Doctors
The day of seeing the Pain Clinic arrives. I have been researching latest treatments and I find one that seems really promising in terms of pain relief – infusions. I print off the latest studies to take with me.
I also take a list of medications/treatments tried and my diagnosis list. My mind usually goes blank when I’m asked, so it’s helpful to have to hand. My heart sinks a little when he asks about treatments I’ve tried – all the standard alternative and normal – physio/hydro etc and then follows up with ah, that’s a shame, you’ve tried everything I was going to suggest.
I want someone with flare! Imagination! Pain is unique and different for everyone, and if you can’t handle someone whose tried acupuncture already and found it unhelpful, then I’m going to struggle with that. So I bring him back to my main reason for referral – facet joint injections. My one last remaining hope.
But he, sadly, is not hopeful. He explains that normally they’d help (normally, normally – I hate that work. Normally surgery would work, normally treatment would work, but with you…) but because of my condition – my whole spine isn’t being held in place properly. If he injected the main site of pain, it’s highly likely that immediately the sites above and below would become the problem instead, so I’d want injections there, and then immediately the next sites would go… and so on.
I then ask about the infusions and he tells me they don’t do them there, and even if they did they wouldn’t be likely to do them to people with Ehlers-Danlos Syndrome as there’s so few of us. Right, so because it’s a highly undiagnosed condition – we deserve to be dismissed.
So my suggested treatment plan is upping my morphine patches until the highest dose possible. If I’m still in pain, then they’d look at the injections. Which will likely make me put on more weight.
The patches have added risks of fatigue, and messing with my hormones (i.e. increasing the acne I already have from using the patches.)
That’s it. That’s my whole treatment plan.
I then explain how helpful I find massage, but I’m worrying about how I will afford it when I finish work at the end of March. He agrees to write in my letter that I need massage as a treatment, which my GP should then be able to set up.
So, it seems this is my life. Painkillers on top of painkillers.

Credit to Kurhan

by The Chronic Chronicles | Jan 30, 2013 | Diagnosis, Doctors, Hospitals
The next step in my quest for facet joint injections, is my GP. But this time when I tell her what I need, she hesitates. Normally she would send me to the local Pain Clinic, but she’s aware my opinion of the clinic is somewhere around… mud. And that’s being polite.
But there must be other pain clinics, right?
So she has a look on the system and it shows a few I can pick from. There’s a hospital nearby with a reasonably good reputation, and she agrees to send me there. She tells me she’d be really interested to know how I get on with them, as it would be great to have an alternative to send people to. Translation: she has issues with the local pain clinic too, but can’t say so.
I’ve been seeing the pain clinic for some years now, and I have to say the treatments/suggestions they offer haven’t changed a bit. The latest medications, research and techniques don’t seem to reach them, so I’ll be really interested to see what the new clinic has to say.





