by The Chronic Chronicles | Jan 8, 2014 | Hospitals, Treatment
I have pain all over the place, but ranking at the top of the list is my lower back. I’d previously had facet joint injections in my neck and shoulders some years ago, but they didn’t help. However, it was before I’d had an MRI (as it took around 8 years of arguing to get one) and so the consultant was ‘guessing’ at what the issues were. Later on the MRI did clearly show an area in my lower back that had degenerative lumbar disease in the facet joints, arthritis, and others issues. It made a much better target for injections than anywhere else, so I thought it was worth a try.
It took another few years of me arguing for them (nothing ever just seems to just happen on the NHS!) After getting nowhere locally, my Ehlers-Danlos specialist at the Royal National Orthopaedic Hospital at Stanmore sent me to see her Pain Management college, who gave me the go-ahead for bilateral lumbar facet joints at L4/L5 and L5/S1 (so four in total).
A few days passed after being told I could have them and suddenly I thought – what the hell am I doing fighting to have needles put into my spine?! I was sedated during my previous injections, but I did have some memories of the procedure. I remember my consciousness kind of returning and thinking ‘please stop now.’ I was later told the sedation didn’t actually knock you out, but simply wiped your memory – and that you would be aware of what was happening as they did it. This memory built up in my mind until I was convinced I’d be strapped down with horrible painful injections into the middle of my spine, then I’d just forget afterwards so I didn’t realise how awful it would be. So I was about 500 times more nervous for these injections than previously.
The whole topic became a ‘do not discuss’ subject. As soon as I thought about it I went into a state of panic, so there was no research done as I normally would, and I didn’t even allow my mum (who accompanied me) to talk about our arrangements of getting there until the day before. I just wanted to block it totally from my mind.
We travelled to Stanmore the day before for two reasons. The first that I can’t make the journey there and back in one day, and the second was that my admission time was 7am. Ugh!
Although I wasn’t having general anaesthetic, I was told not eat after midnight, and no drinking after 6am. It was the latter I’d struggle with as I’m constantly thirsty.
I arrived at the hospital a couple of minutes before 7am and had a choice of parking for the first time ever! When we reached admissions there were a few people waiting outside, but when the queue got the doorway I realised the room was packed with both people queuing, and waiting in the chairs. It wasn’t the easiest getting my wheelchair in and out with no room for manoeuvring. There was only one member of staff dealing with everyone. The older lady in front of me didn’t speak any English, and was soon joined by an interpreter. The staff member made a phone call and I heard him say, “Are the wards still closed, there are a lot of patients here?” He then informed the interpreter they had a bit of a wait ahead. I was next, and was told the same thing.
I was a little cross, only because getting somewhere for 7am isn’t very easy for me and more importantly 7am = grumpiness! I did later found out the wards were opening for the first time after being closed for two weeks over Christmas – so I assume the delay isn’t normal.
I reached the ward and was met with a number of friendly nurses and health care assistants who welcomed me, and showed me my bed. The lady with the interpreter was in the bed opposite me. A nurse admitted me with a huge pile of paperwork, most of which seemed irrelevant in my case! I was asked a couple of times if I had any allergies. She then took swabs for MRSA and then took my blood pressure (which I hate, as it’s very painful. The muscles in my upper arm are very tight and particularly sensitive). I was told I was third in the queue – and the doctor would be seeing me beforehand.
A couple of other patients got in the bed and went to sleep, which seemed like a good idea – and would also make the time pass. However every time I was about to drift off I was woken by someone. The first to measure me for pressure stockings, then again to tell me I didn’t need them. Then a doctor who was working with my consultant arrived to explain the procedure. I was glad it was her and not my consultant as she was much warmer than my consultant is, which helped. She spent a lot of time explaining how much time they took to sterilise everything to reduce any chance of infection. I wanted to rudely interrupt and say that at that point, I didn’t care – I just wanted her to promise she’d knock me out! She then went through the possible risks – infection, numbness in the legs, pain flaring up afterwards and in a very tiny amount of cases nerve damage. She asked if I had any allergies.
Finally I could ask the one thing I wanted to know.
“You will be sedating me, right?”
“Did you ask for it before?”
“Yes,” I emphasised.
“Then we will.”
“Will I know what’s happening?”
“Well, some people do sleep.”
“Please make that happen with me. Please.”
Then the pharmacist came to take note of my list of medications, and asked whether I had any allergies, then a number of nurses came to tell me, “It won’t be much longer.” Then that they were on their way for me, only to still be there sometime later!
Eventually the porters did arrive and wheeled me into theatre. A nurse went through the final questions – checking I knew what procedure I was having, if I’d had any before, if I had any allergies and if it was definitely my signature on the consent form. The nice doctor then fitted the cannula into my hand, before I lay down front-first on the table. They put an oxygen mask on me, a clip onto my finger to measure oxygen (I’m sure that has a proper name) then to my annoyance – a blood pressure cuff which I was told would be taking my blood pressure every few minutes. It took it twice, before I told the nurse how painful it was. “No problem,” she told me cheerfully, and moved it onto my leg instead which was much better. She then began chatting to me about my hobbies and jewellery making, before my consultant began putting the sanitising fluids on my back. The nice doctor then began to input two injections of sedation into the cannula. I closed my eyes – trying to relax. She then asked if I could still hear her, and I said yes. She thought I’d gone to sleep, and I said I hadn’t felt any sedation yet. She said she’d keep going, and added two more tubes.
The next thing I remember is feeling a bit of pain in my back, and a nurse telling me it was all over. I definitely hadn’t been aware of it. I was taken into recovery for awhile, still very sleepy and groggy. A nurse chatted to me for awhile, and I remember telling her to say thank you to the nurses, as they’d calmed me down a lot beforehand. She promised she would. She then asked if I knew which ward I’d been in.
“It began with J…” I answered.
“Jackson Burrows is the only ward beginning with J.”
“No, it wasn’t that. Was it Diane something?”
“I guess now wasn’t the best time to test your memory?” she laughed. She then came back and said that unfortunately they’d moved me to Margaret Harte Ward. I began to worry if anyone had told my mum as I knew she was planning on getting a cup of tea while I was in the theatre (as she’d very kindly not eaten/drunk anything in front of me while I couldn’t).
As the porters wheeled me out of recovery, the nurse suddenly called for them to stop. She dug through a cupboard, and pulled out another blanket to put around me. “Sorry,” she said to the porters. “I just didn’t want her to get cold on the way back.”
When we got back to the ward I spotted my mum very quickly and realised it was the ward I’d been in all along! The nurse handed over to the ward nurse, and said that my blood pressure had risen quite a bit during the procedure, so they needed to keep an eye on it. Argh, more blood pressure checks!
I was left to sleep for a bit as I slowly came round. A nurse then came round to do the blood pressure test. I admit I groaned, and said the test was hurting quite a bit, then of course after gritting my teeth the machine malfunctioned. Just one more time, I was told. Luckily it was back to normal, and as she took the cuff off she realised lots of red marks had come up all the way round (which are still there today!). She gave me an apologetic pat. I asked if she could take my cannula out as it was pulling quite a bit. She took a look and said it was quite red, and that someone would do it before I left. (Well, one would hope so!)
I was told to stay until lunch time, and then I would be discharged. The nice nurse who admitted me then walked past and so I asked her about the cannula, and she said no problem and took it out. She also checked my ‘wounds’ (just slightly larger than needle marks) and said she was happy with how they looked.
Still waiting opposite me was the older lady with the interpreter. I heard a nurse say to her that her operation wasn’t going to be until mid-afternoon – yet she’d been admitted at 7am! It seemed mean to make her wait so long, and I assume the NHS had paid extra for the interpreter when they could had admitted her at the 11am or 2pm admission times. I noticed the little old lady chatted non-stop to her interpreter, which made me smile as I could just imagine in the 7+ hours the interpreter sat with her she got to hear her entire life story.
I left at 1:40pm, slept all the way home, slept all afternoon and very unusually for me – all night!
So all in all – it wasn’t nearly as bad as I dreaded. The staff – particularly the nurses, were lovely. There were lots of touches of kindness, like the nurse in the theatre distracting me from my nerves, the recovery nurse chatting to me as I came round and making sure I was warm, and the staff back on the ward who took care of me and offered me toast and regular drinks when I came round. They all made it a much easier experience. Also – the NHS really, really want to know if you have any allergies.
I’m in a lot of pain now which feels different to my usual pain. I was warned I may flare up, particularly where the needle touches the bone – so I’ve no idea if it worked yet. I think I need to wait for all of that to calm down over the next couple of days before I can tell if it helped.

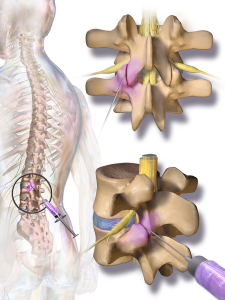
An image of a facet joint injection

by The Chronic Chronicles | Oct 30, 2012 | Diagnosis, Doctors
For so long now I’ve been trying to get an MRI, after my mobility vastly reduced over the past few years. Luckily my specialist consultant agreed, and asked my GP to get one done locally.
My GP told me it showed a few issues
- Limited marrow oedema (degeneration in the joint cartilage) in L2
- Moderate degenerative changes at L4/5 and L5/S1.
- Moderate sized disc bulge at L4/5 which along with ligamenta flava hypertrophy (enlarged connective tissue) caused by facet joint arthritis on both sides, which has resulted in acquired central canal narrowing (12mm instead of 16mm)
- L5/S1 moderate broad based disc bulge causing an indent in the thecal sac. This has reduced the central canal measurements from the expected 17mm, to 11mm.
- Synovial cysts are on both sides of the facet joints at L5/S1 level.
However, locally – I’m still getting nowhere. My GP referred me to a spinal surgeon to discuss this, but in my area we have a ‘spinal pathway’ – seemingly controlled my physiotherapists. Even having my results upfront, they still want a physiotherapist to carry out a physical assessment, which isn’t going to tell them anything!
After waiting eight weeks for this, I went back to my specialist consultant at the Royal Orthopedic Hospital, who agreed to refer me to a surgeon there, so I can actually discuss my options (if any).
But, it at least explains why I can’t walk far – both the spinal narrowing, and facet cysts would cause this issue and can’t be solved with the hand wave ‘just exercise more’ than doctors love.

English: MRI sagittal image of sacral and dorso-lumbar perineural cysts (Photo credit: Wikipedia)

by The Chronic Chronicles | Sep 10, 2012 | Diagnosis, Hospitals

I was told me to get to the hospital at about 5 to prepare for my MRI at 5:25pm.
I immediately began to be concerned – I was having a high pain day, and one problem with an MRI, for those who are new to them – you have to keep completely still. If you move they will start the whole thing again. And anyone who knows me (or anyone with chronic pain!) will tell you – I can’t keep still. I personify a fidgeter.
I took every painkiller I could, and arrived at 5pm, parking in a blue badge space next door to the MRI centre, which was a great bonus as they were normally full. This meant I didn’t have to faff around getting my wheelchair out, as I was literally two steps away.
I was given paperwork to fill out, and immediately had to answer yes to a ‘red flag’ question – are you wearing any medicine patches? The lady informed me I would have to take it off. Oh. You mean the patch that was brand new on that morning, that’s meant to last me another four days and if I take it off means I will run out of patches four days early, causing mayhem to my delivery system, and will leave me without lovely morphine pumping through me at a time I need to lay down for half an hour and keep still? Apparently one person once had a reaction and it burnt her, so they now have to be taken off. I’m not moaning at this policy – I just wish they’d have mentioned it as I would have held off putting it on and wasting £70 worth of patch.
I’m then informed I’m in the mobile scanner, which is on the other side of the car park. At the look on my face, the receptionist kindly offers to call me a wheelchair, and I take her offer thankfully. At 5:30pm a lady arrives, who has a limp, and is told she needs to find me a wheelchair. She returns dragging a battered looking thing which she can’t get to move. She limps off to find another wheelchair in the hospital – and returns with a chair that needs to be pulled backwards. The rain is now pouring down, and I look longingly at the people going into the next room for the MRI as I’m pulled out the room backwards, by a lady who looks like she needs a wheelchair too, into the wet, cold car park.
We don’t make it very far – she pulls me straight into the tunnel that joins the two parts of the hospital up, and then says she is going back for an umbrella, and leaves me. A grumpy looking security person comes along and closes all the doors around me, before I can protest. Limping lady arrives back and isn’t happy that she now has to try and get a wheelchair through a couple of sets of closed doors. Her umbrella blows inside out, and she gives up. The receptionist appears and takes over the pulling duty, and they take me to the other side of the hospital. Lucky for them – I can walk a few steps, because the mobile unit they have sent me too isn’t accessible. I’m told to stand on a lift in the pouring rain – which isn’t big enough for a wheelchair, and they send me up. I get even more soaked and cold while she shouts through to the other side to try and explain how they open the door to someone who can’t find the button.
I’m shaking by the time I get seated next to the person taking images, and can see the outline of a pelvis on the screen. They are all sitting in coats, and look cold and bored. I’m nervous – I’m soggy and about to go into a big electrical machine, but the lady assures me it won’t electrocute me! I’d spent the afternoon putting together a ‘relaxing music for an MRI’ CD to try and drown out the noise, so I get it out, but they tell me the CD player is broken. I’m struggling to breathe by now as panic sets in, so I puff on my inhaler before they take my bag away to lock up, and I take my patches off. I’m not scared about the MRI itself – just worried about them having to restart because I move. The other lady finishes and is getting dressed. I’m aware of this as the porter walked in on her doing so without knocking.
I’m ushered in next, although I’m told I can’t take my stick in and will have to use the bed to lean on – which is too low to be possible. It’s small and cramped. The lady with me doesn’t really speak English very well, and waves at the bed, and then raises it until it’s much too high for me to get on. She then sighs and says I was meant to sit on it first, but I hadn’t caught on what the random wave towards it meant. I have to take off anything that includes metal – but luckily I dressed to avoid zippers, etc. She tells me to lay down and put the ear plugs in. Every time I put them in, she then asks me a question – so I have to take them out, only for her to be asking if I’m ready.
She sends me through into the narrow tunnel, before she stops and says ‘Are you arms touching the sides? They are. She seems concerned, which makes me concerned – but she says, ‘Oh, I’m sure it will be fine. Just hit the emergency buzzer if you feel anything.’ She then leaves, and I’m wondering if I feel what?
A voice comes over the intercom to say they are starting, and I cannot move. I’m completely tense – they haven’t given me more than a couple of seconds to try and relax out and get into a comfortable position, and it’s off before I can do so. I then have to maintain the completely uncomfortable position – my muscles trembling and spasming, in my fear of moving and making them restart, therefore prolonging it.
I’m also worried about my arms. The time before I had an MRI I just tried to daydream, but this time my focus is on where my arms are touching the top. As the tube begins to warm naturally – as anyone would in a narrow tube, I worry about her definition of warm. Does she mean any kind of warmth, or if I actually feel it start to burn? I get hotter and hotter in there, probably as I panic.
I’m so glad when it’s finally over. They drag me back to the MRI centre in the backwards wheelchair, and leave me to get back to the car. Unfortunately I’m left feeling so dizzy, sick and in agony, I shuffle back to the car and almost collapse in. I’m left in excruciating pain for the night, even after replacing the patch.
So, that was my experience of my second MRI. I just hope it’s all worth it!
Next up: the results are in…

by The Chronic Chronicles | Sep 9, 2012 | Diagnosis, Hospitals
The first part of the story can be found here. From 2008 onwards my mobility vastly decreased. I swiftly went from sticks, to wheelchairs, to sometimes a few steps being too much. The chiropractor I was seeing at the time advised she thought my facet discs may be getting worse, but wasn’t entirely sure.
By this point I had a diagnosis of Ehlers-Danlos Syndrome, was aware one of the issues is that it causes joints to degenerate a lot quicker than they should as they are hypermobile and moving out of place all the time, which then in turn causes them damage. So it’s sensible to keep an eye on it, as you could technically end up crumbling away!
Last year I brought up this issue to my GP. While I understood and generally accepted the condition, and the general levels of constant pain, I was worried about what was going on in my lower back which has been the worst pain I have for some time. She agreed with me it was a valid concern, but said she did not have the authority to send me for an MRI unless it was for a surgical reason. I pointed out that I was unsure if it was surgical until it was scanned, but as she could find no symptoms relating to a disc pressing on a nerve – which is not my worry anyway, there was nothing she could do.
Instead she wrote to my two EDS specialists. One my specialists I really like – he listens in appointments, and makes lots of referrals. The other one comes across as slightly dismissive, and mostly spend her time trying to get me to lessen my painkillers – which wasn’t going to happen, after finding my current regime the best I’ve had so far. The problem with the first specialist is that he doesn’t seem to respond to GP letters. I realise he’s busy, and should have retired years ago – but local doctors just don’t have the skills and knowledge to treat EDS most of the year, and we shouldn’t have to wait for a check up just to get a simple question answered.
The second specialist did come back, however – to say she felt the answer to my issue was exercise. I have to say my letter back her from my GP and I wasn’t particularly polite. Oh, exercise! Silly us! I’ve done all the bloody stretches and exercises they have given me, and it’s ten years later and my lower back is simply getting worse. This is not an issue to simply dismiss as ‘have an exercise sheet.’ I have to say all my trust in her immediately evaporated at that response.
My GP then tried again to a local Pain Consultant. I have to say I’ve never liked this pain consultant. I saw him before I had a diagnosis, and he seemed to immediately take against me because I’d already tried the suggestions he normally makes to patients (acupuncture and a TENS machine… Yep, that’s it.) On my first appointment I asked him if he thought it may be Fibromyalgia, and he responded, “You can call it that if you like, but I don’t as it’s too American.” On my second appointment he said I was on too many painkillers, and that I needed to come off one of the painkillers. On my third appointment he said I wasn’t on enough painkillers, and upped my morphine dose.

But I still wasn’t expecting the response I got back from him that stated in black and white that to give me tests/injections into my spine would be “medicalising her condition, when she should be seeking psychiatric help” or something to that effect. He also seemed to have forgotten I have a diagnosis Ehlers-Danlos Syndrome, and stated my condition was Chronic Pain Syndrome instead.
Luckily, my follow-up with the first specialist was due a few months later – and he agreed with me I should have an MRI, as we don’t exactly know what the issue is – whether it’s something that’s got worse, or something new. The bad news is that they are transferring existing EDS patients from my preferred hospital of UCL London, to Stanmore – therefore losing him as my specialist, and making the other one my primary.
Two weeks ago my GP phoned to say now that my consultant has agreed in regards to the MRI, I can now go on the waiting list! I wasn’t sure how long they were taking, and hadn’t heard anything when couple of weeks ago I received a phone call from the MRI department asking if I was aware I had an appointment in a couple of hours, as I had yet to confirm it. Um, no, I certainly did not. I thanked her profusely for calling me, if she hadn’t I would have gone down as a Do Not Attend – and gone to the back of the waiting list at best, discharged at worst.

by The Chronic Chronicles | Sep 8, 2012 | Diagnosis

My path to a diagnosis was a long one.
I seem to have had a few people in my life at the moment develop back issues. In all, or at least almost all cases they seem to have gone to their doctor, been sent for an MRI, been diagnosed and sent for treatment. That’s brilliant, exactly how the NHS should be.
That’s not how it’s been for me. Sorry to bore those who’ve heard this before, but 10 years ago I started to get a strange pain in the joint between my neck and spine (that one that’s a little bump.) It began to crack, and feel really stiff. The pain spread into my shoulders and upper back. It then went into my lower back – badly. I began to not be able to stand as long as I used to, or sit comfortably. I fidgeted constantly, and my joints all began to loudly crack all the time. I didn’t know what the hell was wrong with me. The first rheumatologist I saw said I’d grow out of it. The second said it wasn’t arthritis, but didn’t know what it was. The next said I had bad posture – ignoring the fact I was hunched over due to the pain.
In the years between 2002 and 2008, that pain spread into every joint, every muscle. The fatigue was getting worse. I could only walk for short periods of time. I saw rheumatologist after rheumatologist, and two different pain consultants. Each time I raised the possibility of an MRI, but it was dismissed.
I finally saw a third Pain consultant in 2008. He was an asshole. It was the first time I left a consultants room in tears. He told me there was nothing wrong with me, and he said he would prove it by sending me for an MRI.
I was pissed off, but also pleased. At least his bad attitude was getting me an MRI. When I returned I saw yet another pain consultant who told me the MRI “showed nothing.” I was very disappointed. It’s very hard to be in constant pain and have no idea why. You hope it does show something – because at least you know, and then you can look at possible treatment options.
I continued to see the spinal specialist physiotherapist at the hospital who was able to print a copy of the MRI off for me. The same physiotherapist who said, “You are hypermobile as hell. I can tell just by looking at you.” She didn’t help me physically, but she tried – and helped point me in the right direction of my final diagnosis.
Unfortunately, despite having a copy of the MRI, I didn’t understand a word of it. A few months later I sat, although I can’t say why it took me that long, I sat googled every single word of the MRI that ‘showed nothing’ and was surprised to find various disc bulges in my lower back and neck, quite bad facet disc degeneration and arthritis in my lower back. So there was something. It might not have been the worst MRI he’d seen, or not operable – but I believe I should have been told what it did say.
From 2008 my mobility continued to go downhill, first causing me to walk with a stick, and later needing a wheelchair more and more often. My lower back continued to decline; at best feeling like someone was gripping into it, crushing and aching. At it’s worse? Well, there aren’t really words. I was desperate to find out what was happening, but it took another four years to get that update.






