
by The Chronic Chronicles | May 30, 2015 | Daily Life
I had so many plans for May – which is Ehlers-Danlos Syndrome awareness month, and it’s just all gone by in a flash of bad health, hospital appointments and glass making.
Fused glass making is a new hobby I’ve got into, and I’m really enjoying it. If you’re interested in seeing my new makes I have a facebook page and a Folksy shop (the UK equivalent of Etsy). I’m also running a competition to win a Dotty Suncatcher at Facebook as soon as my page reaches 100 likes. It’s difficult starting a new page from scratch, so any support there would be really appreciated.

Teal Dish with Clear Detailing, Spotty Suncatcher and Black and Gold Pendant
I’ve been making jewellery for awhile, and have wanted to try glass making as something that would go nicely with it (i.e. making pendants/jewellery out of glass), but also being able to branch into something different like dishes, candle holders, etc. I find the jewellery making market quite saturated, and difficult to stand out. Not that I would ever be well enough to make a business out of my crafts, they all remain hobbies, but it’s still nice to sell the odd thing to be able to pay for my glass or beads!
I’ve spent most of my month having medical appointments, including having some awful tests on my bladder – which I will never ever have again. They all came back clear for blockages/cysts, which means it’s down to spasms probably caused by the Ehlers-Danlos Syndrome, so the next step will be medication.
I’ve also been to Cambridge to visit the biggest sleep specialist clinic in the UK. I’ve had problems with my sleep since I was 15 – from severe bouts of insomnia, sleep patterns all over the place, horrible levels of fatigue, day-time sleepiness, and unrefreshing sleep. I got put in the wrong clinic – I should have seen the consultant as it’s the EDS causing the problems, and the autonomic dysfunction and adrenaline issues that go along-side the condition. Instead I got put in the nurse-led insomnia clinic, where they give sleep hygiene advise, such as go to bed at the same time, have a dark room, etc. I know. I’ve had this problem for twelve years, I’ve tried all the basics. This visit was an end-of-my-tether, absolutely desperate need for real medical help. Luckily the nurse did seem to understand my point, so I’m going back next month for a sleep study test which will hopefully be a start, at least.
For the last year I’ve been trying so hard with exercises tailored towards my condition. For sometime I’ve stumbled along seeing physiotherapists who know nothing about my condition, and having a six-week block of hydrotherapy every few years. So sometime ago I decided to put my foot down, and get some real help.
I found a physiotherapist who specialises in EDS, a rarity indeed. His clinic is in another town, but the way he does things means I don’t have to visit that often – he gives me lots to keep going on my own, and does progress checks. I also started doing 1-2-1 Pilates sessions. I’ve tried this a few times – joining a class, or going to the physiotherapy-led Pilates sessions at my local hospital. Both were total disasters, and were aimed at people way healthier than me. Even the hospital ones which I thought were for people with injuries were awful – as most people in the sessions had one problem area – a bad knee, a bad shoulder. Sadly that’s way above my level, as I can’t stand for more than a few seconds, and have problems with every joint and muscle group. So I would just end up half-collapsed in the corner, rather than having effective assistance.
1-2-1 has been great – the instructor has tailored everything towards my condition and problem areas. It’s all on the mat, so no standing at all – and she breaks everything up so I’m not concentrating on one area for too long, which always leads to a flare up. What I do is very basic compared to a healthy person, but between the physiotherapy, pilates and more regular hydrotherapy, I’ve had lots of improvements physically – more muscle control and strength. Sadly it’s not translated into any pain relief at all, which has been incredibly frustrating as that’s obviously why I’m doing it. No one can tell me why it hasn’t helped in this way, but I’m not going to give up – although it really should have helped even a little by now, so I’m not sure it ever will. Hopefully it will stop things getting worse, and help prevent additional injuries though, so it still has a place.
My last piece of news, good this time, is that I’ve now completely given up my huge vice – Diet Doctor Pepper for just under six months. I’ve been trying to kick that habit for years, so I’m thrilled. I’m now a water and ice kinda gal.
So that was May. Hopefully June will bring more glass making, less medical appointments and lots of warm weather.

by The Chronic Chronicles | Jan 9, 2015 | Doctors

Credit to Kurhan
Yesterday I went to London to see Dr Hakim, one of the top specialists in Britain for Ehlers-Danlos Syndrome.
I was nervous when I got there – I always am before I see a consultant, due to many, many bad experiences. However he immediately put me at ease, and was a nice, approachable person.
I’d made a list of problems I wanted to talk about, and he made a note of them and went through each in turn giving me ideas and suggestions of particular treatments or medications I could try.
He said in terms of exercise I was doing everything right, and everything I could. This meant a lot, as I’ve had medical professionals be so judgmental with no understanding of how hard it is to do the ‘little’ I do without putting myself in bed for weeks. I told him what one Pain Consultant had said – that I should be exercising six times a day. He said it was such an easy thing to say, and proved how little he knows.
We spoke about my Physiotherapist Leon Stephens at Sudbury Physiotherapy Centre who specialises in Hypermobility, and has been great, and Dr Hakim knew of him, which was good.
At some point this year I need to renew my Employment and Support Allowance, and in the next couple of years my indefinite Disability Living Allowance award will be changed over to the replacement – Personal Independence Payment (PIP). I’m terrified about both of these, as are most disabled people in the country who currently rely on them – or may need them in the future – to survive. I never know how people may react to something like that, due all the ‘scroungers’ rhetoric in the media, that has been picked up by so many.
Since I received my diagnosis letter in 2011 – I haven’t had a decent letter from a consultant that I could use as medical evidence. I’ve seen lots of consultants, but letters are generally of the “Treatment x didn’t work, been discharged” variety which won’t help much in terms of summarising where I’m currently at on the whole. I feared the lack of letters may go against me, as the Department of Work and Pensions will argue I can’t be that bad if I don’t see a consultant regularly.
Dr Hakim was very understanding of this, and we spoke at length about the PIP changeover, and he knew how hard it was on his patients. He said it’s obvious the reason I don’t have new evidence is because I’m doing the best I can at home to manage, but he would write an updated version for me to keep on file for when I need this.
This will take a huge worry away from me, so I’m thrilled.
He recommended that I take a multivitamin daily – he mentioned the Well Woman one, to make sure I’m topping up on anything that could be contributing to my levels of fatigue. He’s also going to ask my GP to check every blood test has been done, including the T3 Thyroid test that the NHS often miss out. He also suggested getting some Melatonin from the US, as well as suggesting some other sleep and pain medications I have yet to try that he’s going to suggest to my GP to look into (I can’t remember the name of them currently!) He also recommended some consultations in other fields that I could see if I continue to get nowhere locally.
He also suggested that anyone with POTs or autonomic dysfunction (including sleep problems) to drink an Isotonic drink called Nuun. He explained that they tell people like us to keep hydrated, so we drink water – but it actually make things worse as it dilutes the salt in our blood, so our kidneys then filter it and we pass it out with urine leaving things actually worse. (Or something like that!)
So he suggested drinking a salt isotonic drink which means that we are really hydrated, as drinking liquid with a similar salt content as our blood means it will do its job, rather than being filtered and disposed of straight away. Most of the similar products on the market i.e. sports drinks, Lucozade, etc are full of crap and sugar, so he suggests Nuun as it doesn’t add much else, just some flavouring. He suggested at a minimum to drink one before bed, and one as soon as you wake up, and this should stabilise some of those issues.
They are pretty expensive, but we only need half a tablet at a time, as the whole tablets are designed for athletes.
We also spoke about Prolotherapy, which is a new therapy I’m hearing a lot about recently, mostly from Americans, and I was interested in his thoughts. He said there was no evidence for it, and some of his patients had been made worse by it.
I found Dr Hakim very understanding, kind and obviously knowledgeable. All in all it was a great appointment – and when his letter arrives I will add anything helpful I’ve forgotten!
Professor Grahame retired from NHS patients some time ago, and is no longer taking on new private patients. I believe he may still have a private clinic for under 16s, but Dr Hakim is a perfect alternative.
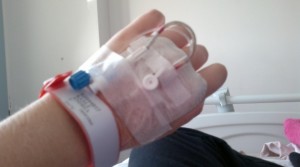
by The Chronic Chronicles | Dec 23, 2013 | Hospitals
I stumbled across the treatment of ‘infusions’ sometime ago, and then kept seeing them being mentioned. I began to try to find out more about them, but information was limited.
I was aware it usually consisted of either Ketamine or Lidocaine being given by an IV, and for some it works really well for pain relief. For others it seems to do nothing at all.
Eventually a friend kindly offered to search the academic databases he had access to and sent me all the research he could find. They were generally all positive.
‘Intravenous Lidocaine: An Outdated or Underutilized Treatment for Pain?’ by Gary McCleane stated, “The drug is administered over a relatively short period of time and yet the potential relief lasts significantly beyond both the period of administration and the plasma half-life of this local anesthetic.” He goes on to state that, “an infusion over a few hours can produce relief that extends to weeks and even months. Consequently, side effects, if any are apparent, are short lived and last for a much shorter time than the pain relief.”
McCleane explained that for many patients undertaking this treatment it becomes their only form of pain-relief, and they’re able to stop all other medications for pain. A trial of 82 patients found that 82% had a very good pain reduction after their infusion. In a second study on people with Fibromyalgia it was found that 40% of patients had between 13-18 weeks of relief.
A second study called ‘Efficacy and adverse effects of intravenous lignocaine therapy in fibromyalgia syndrome’ concluded that the therapy “appears to be both safe and of benefit in improving pain and quality of life for patients with fibromyalgia.”
The one downside is that there wasn’t much research on the therapy, and when a study had taken place they had very small sample sizes. There are also side effects such as hypotension, tachycardia, infections and other such fun times.
I began by asking my GP about them, but she’d never heard of them. I asked at the various London hospitals I’m under, but was told they didn’t do them. I came across a number of people with Ehlers-Danlos Syndrome who’d had them, but it was never at a hospital near to me.
I then visited a pain clinic in another town but they too stated they didn’t do them, and if they did they wouldn’t do it for Ehlers-Danlos Syndrome as there weren’t enough of us with it. (Red flag to a bull!)
I then changed GPs, and she too hadn’t heard of them – but a few weeks later I got a phone call from her. She explained she’d just had a patient in to see her who’d just had infusions at the hospital in my own town! She told me to come and see her, and she’d get me referred.
I saw a consultant at the pain clinic last week and she agreed I could have one infusion. I’m not sure why just one, but still it’s good news!
I’m also due to have facet joint injections in January, so there are two treatments coming up that allow me to have some hope.

An IV
Credit to: andyk

by The Chronic Chronicles | Jan 20, 2013 | Daily Life
I can’t drive far, so it means my poor mum has to drive me to hospital appointments, and she HATES driving in central London. She’ll do it, unlike a lot of people, but it’s not fun.
It’s already a worry before we leave that we’ll get to the hospital and they’ll be no parking. This has happened loads of times before, and usually results in madness and mayhem. And that’s putting it lightly.
Picture this: last hospital appointment at the University College Hospital in London, which has six blue badge spaces. We’d been stuck in traffic and were now 45 minutes late for the appointment and of course all six spaces are taken. So we pull up outside, put the wheelchair together and mum sends me on my way while she goes to hunt for a space. Wheelchair battery promptly dies, so I’m having to use my feet to pull the wheelchair along (Fred Flintstone style) at 0.000000000001 miles per hour. I’m given the wrong directions and head to the other end of the department, before being sent back, and arrive at the nurses station way, way past my appointment time and promptly burst into tears and have a mild panic attack. Luckily, they took pity on me and they let me see the consultant at the end of his surgery time.
So parking, and being able to have someone with me? Helpful. Anyway, as a passenger in a car, I have an unfortunate issue of falling asleep. I’m generally close to exhaustion at all times, and there’s something about a car I obviously find soothing, as I can’t fight it and within a few minutes I’m usually out of it.
However, my mum struggles with the whole driving in London thing and trusting the sat nav, so I get woken up every 15 minutes with increasing franticness, “Which road do I take?” I mumble an answer, and then go back to sleep again. This apparently stresses her out, and she’d rather have an awake passenger when going to London. Whoops.


by The Chronic Chronicles | Oct 30, 2012 | Diagnosis, Doctors
For so long now I’ve been trying to get an MRI, after my mobility vastly reduced over the past few years. Luckily my specialist consultant agreed, and asked my GP to get one done locally.
My GP told me it showed a few issues
- Limited marrow oedema (degeneration in the joint cartilage) in L2
- Moderate degenerative changes at L4/5 and L5/S1.
- Moderate sized disc bulge at L4/5 which along with ligamenta flava hypertrophy (enlarged connective tissue) caused by facet joint arthritis on both sides, which has resulted in acquired central canal narrowing (12mm instead of 16mm)
- L5/S1 moderate broad based disc bulge causing an indent in the thecal sac. This has reduced the central canal measurements from the expected 17mm, to 11mm.
- Synovial cysts are on both sides of the facet joints at L5/S1 level.
However, locally – I’m still getting nowhere. My GP referred me to a spinal surgeon to discuss this, but in my area we have a ‘spinal pathway’ – seemingly controlled my physiotherapists. Even having my results upfront, they still want a physiotherapist to carry out a physical assessment, which isn’t going to tell them anything!
After waiting eight weeks for this, I went back to my specialist consultant at the Royal Orthopedic Hospital, who agreed to refer me to a surgeon there, so I can actually discuss my options (if any).
But, it at least explains why I can’t walk far – both the spinal narrowing, and facet cysts would cause this issue and can’t be solved with the hand wave ‘just exercise more’ than doctors love.

English: MRI sagittal image of sacral and dorso-lumbar perineural cysts (Photo credit: Wikipedia)






